Call to action for stronger, better-funded federal nutrition research
Released July 20, 2020
Experts and coalition call for better coordination to prevent costly diet-related illnesses and better address food insecurity while accelerating discoveries, economic growth, and improving public health and population resilience.
Co-authors are former USDA and NIH policy advisor Sheila Fleischhacker, former USDA Undersecretary Cathie Woteki; former director of the Office of Dietary Supplements Paul Coates; former NIH Division of Nutrition Research Coordination and Associate Director for Nutritional Sciences Van Hubbard; MS/MPH candidate at the Friedman School of Nutrition Science and Policy at Tufts Grace Flaherty; former USDA Secretary Dan Glickman; former Senator Tom Harkin; former FDA Commissioner David Kessler; CEO of The Angiogenesis Foundation Will Li; Chairman of the Department of Medicine and Physician-in-Chief at the Department of Medicine at Brigham & Women’s Hospital Joe Loscalzo; Bipartisan Policy Center chief medical advisor Anand Parekh; NASEM Food Forum Chair and President of SR Strategy Sylvia Rowe;Vice Chancellor and Dean for Agriculture and Life Sciences at Texas A&M Patrick Stover; former executive director of USDA Center for Nutrition Policy and Promotion Angie Tagtow; and Yun Family Foundation’s Joon Yun.
Confused by whole grain labels on food packaging? Study finds you're not alone.
Released August 10, 2020
Researchers say the results provide legal evidence for proposed changes in labeling regulations
The study, led by researchers at the Gerald J. and Dorothy R. Friedman School of Nutrition Science and Policy at Tufts University and NYU School of Global Public Health, is published today in Public Health Nutrition. The researchers say the findings could help lead to enhancements in food labeling.
“Our study results show that many consumers cannot correctly identify the amount of whole grains or select a healthier whole grain product. Manufacturers have many ways to persuade you that a product has whole grain even if it doesn’t. They can tell you it’s multigrain or they can color it brown, but those signals do not really indicate the whole grain content,” said first author Parke Wilde, a food economist and professor at the Friedman School.
Authors are Parke Wilde, Jennifer Pomeranz, L.J. Lizewski, and Fang Fang Zhang
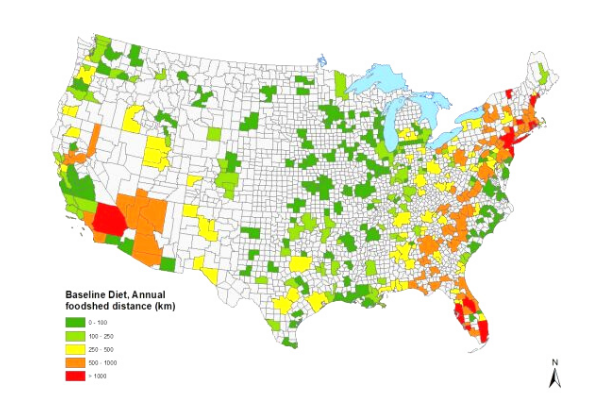
Some but not all U.S. metro areas could grow all needed food locally
Released September 14, 2020
A modeling study found that urban centers in green could feed themselves with cultivated cropland located within an average distance of 250 kilometers (155 miles), but urban centers in yellow, orange and red would need to draw from wider areas.
Under all the diet scenarios, the model projected the United States having a surplus of land for meeting domestic food needs. In the current American agricultural system, some farmland is used for biofuels and export crops. The researchers point out that if metro centers focused on eating locally, many agricultural areas would face new questions about local land use priorities.
Image Credit: Kurtz, J.E., Woodbury, P.B., Ahmed, Z.U., & Peters, C. J. (2020)
Tufts University to lead $100M program to reduce risk of zoonotic viral spillover, spread
Released September 30, 2020
The program leverages expertise from across Tufts’ schools in infectious-disease forecasting, surveillance, prevention, and eradication; food and water safety and risk reduction; social behavioral change; global health diplomacy; and One Health programming and education.
“Part of our mission at Tufts is to make the world a better place, and with this initiative, Tufts and its many coalition partners will make a lasting, positive impact on global health,” said Anthony P. Monaco, the university’s president.
The Tufts schools and centers involved in the program include Cummings School of Veterinary Medicine at Tufts University, the Gerald J. and Dorothy R. Friedman School of Nutrition Science and Policy, Tufts University School of Medicine, The Fletcher School, the Feinstein International Center, and the School of Engineering.
$100k Jean Mayer Prize from Tufts Nutrition awarded for tackling COVID-19 food crisis
Released September 30, 2020
The Gerald J. and Dorothy R. Friedman School of Nutrition Science and Policy at Tufts University is awarding the school’s biennial $100,000 Jean Mayer Prize for Excellence in Nutrition Science and Policy to three organizations for their collective efforts to support food communities and empower individuals through food and nutrition before and throughout the COVID-19 pandemic.
The Jean Mayer Prize honors the legacy of Dr. Jean Mayer, the founder of the Friedman School and one of the world’s leading nutrition scientists who was instrumental in addressing hunger in the U.S. through engaged policy actions. The recipients were the HEAL (Health, Environment, Agriculture, Labor) Food Alliance, the James Beard Foundation, and World Central Kitchen (for its Restaurants for the People program).
New study finds fish oil omega-3s EPA and DHA work differently on chronic inflammation
Released December 7, 2020
The omega-3 fatty acids EPA and DHA work differently against chronic inflammation, according to the results of a small randomized study, suggesting each has its own important role to play in regulating the immune system.
The 34-week trial, led by researchers at the Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University(HNRCA), compared the effects of the two omega-3s in a small group of older adults with obesity and chronic low-grade inflammation. The participants were randomly assigned to receive either EPA or DHA supplements twice a day.
“The jury has been out, so to speak, on how the two major components of fish oil work – and whether one might be better than the other. These results suggest that DHA is the more powerful of the two on markers of inflammation in the body, but that’s not the end of the story,” said Stefania Lamon-Fava, a scientist on the Cardiovascular Nutrition Team at the HNRCA.
So, J., Wu, D., Lichtenstein, A.H., Tai, A.K., Matthan, N.R., Maddipati, K.R., and Lamon-Fava, S. (2020)
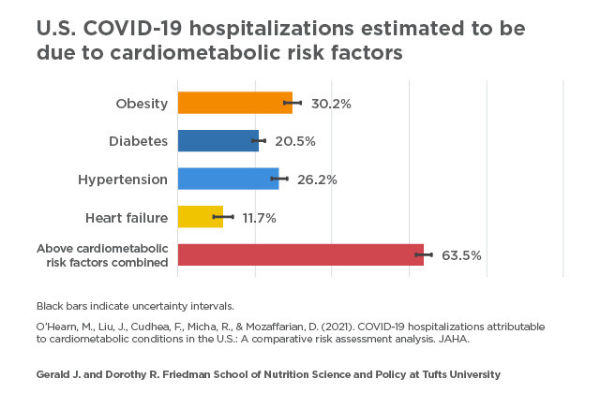
Study Estimates Two-Thirds of COVID-19 Hospitalizations Due to Four Conditions
Released February 25, 2021
A modeling study suggests a majority of adult COVID-19 hospitalizations nationwide are attributable to at least one of four pre-existing conditions: obesity, hypertension, diabetes, and heart failure, in that order.
The study, published today in the Journal of the American Heart Association (JAHA) and led by researchers at the Gerald J. and Dorothy R. Friedman School of Nutrition Science and Policy at Tufts University, used a mathematical simulation to estimate the number and proportion of national COVID-19 hospitalizations that could have been prevented if Americans did not suffer from four major cardiometabolic conditions.
“Our findings call for interventions to determine whether improving cardiometabolic health will reduce hospitalizations, morbidity, and health care strains from COVID-19,” said Dariush Mozaffarian, lead author and dean of the Friedman School. “We know that changes in diet quality alone, even without weight loss, rapidly improve metabolic health within just six to eight weeks.
Additional authors on the study are Frederick Cudhea and Renata Micha at the Friedman School, and Junxiu Liu, a postdoctoral scholar at the Friedman School at the time of the study, now assistant professor at the Icahn School of Medicine at Mount Sinai.
Time to Shift from “Food Security” to “Nutrition Security” to Increase Health & Well-Being
Released April 1, 2021
The Viewpoint published online in JAMA, was authored by Dariush Mozaffarian of the Friedman School of Nutrition Science & Policy at Tufts University, Sheila Fleischhacker of Georgetown Law School, and José Andrés of World Central Kitchen.
The concept of food security focuses on access to and affordability of food that is safe, nutritious, and consistent with personal preferences. In reality, however, the “nutritious” part often has been overlooked or lost in national policies and solutions, with resulting emphasis on quantity, rather than quality, of food, say the authors.
“The current approach is not sufficient,” the authors write, and “traditionally marginalized minority groups as well as people living in rural and lower-income counties are most likely to experience disparities in nutrition quality, food insecurity, and corresponding diet-related diseases.”
Study Finds Americans Eat Food of Mostly Poor Nutritional Quality – Except at School
Released April 12, 2021
Analyzing the diets of about 40,000 adults and 21,000 children between 2003 and 2018, the research team found significant improvements in the nutritional quality of school food consumed over this period, almost all happening after the passage of the federal Healthy, Hunger-Free Kids Act in 2010, which mandated much stronger school and early child care nutrition standards. The findings represent food as actually consumed from different U.S. sources, not what is theoretically available to be purchased.
“Schools are now the single healthiest place Americans are eating. This finding is particularly timely given widespread school closures over the last year from COVID-19, and current efforts to safely and fully reopen schools. Our results suggest substantial nutritional harms for millions of kids who have not been consistently receiving meals at school and must rely on other sources. These harms also disproportionately affect low-income, Black and Latinx children,” said Dariush Mozaffarian, dean of the Friedman School and senior author of the study.